Vaginal Dryness During Menopause
Meta Description: Understand why vaginal dryness during menopause occurs and explore effective treatments, from moisturizing therapies to low-dose estrogen and laser [...]
Read MoreSpinal stenosis occurs when spaces in the spine narrow and compress nerves, causing pain, numbness, and weakness
About 9% of U.S. adults have lumbar stenosis, with risk increasing significantly after age 50
The two main types are cervical stenosis (neck) and lumbar stenosis (lower back), each with distinct symptoms
Diagnosis involves physical exams combined with imaging, such as MRIs and CT scans
Many people manage symptoms successfully with physical therapy, medications, and lifestyle changes
Surgery becomes an option when conservative treatments fail to provide relief
Back pain affects millions of people, but not all back pain is the same. When someone asks what spinal stenosis is, the answer involves a specific condition where the spaces inside the spine become too narrow. This narrowing puts pressure on the spinal cord and the nerves that travel through the spine. This compression can lead to irritation, pinching, back pain, sciatica, and other nerve issues. The condition develops slowly, so symptoms often appear gradually. Some people have stenosis but feel no pain at all, while others experience severe discomfort that limits daily activities. Understanding this condition helps people recognize warning signs early and seek proper care through Doctronic.ai.
The spine is made up of 24 movable vertebrae plus the sacrum and coccyx stacked on top of each other. These bones create a tunnel called the spinal canal. The spinal cord runs through this canal, protected by the bones around it. Between each vertebra, small openings allow nerves to branch out to different parts of the body. Cushioning discs sit between vertebrae to absorb shock during movement. When any part of this system breaks down or changes shape, the canal can become narrower.
Cervical stenosis happens in the neck area and affects the upper part of the spinal cord. This type can cause problems in the arms, hands, and even legs because the spinal cord connects to the entire body. Lumbar stenosis is a common condition of the lower back. Approximately 9% of adults in the United States have lumbar spinal stenosis, and this number increases with age. Lumbar stenosis typically affects the legs and lower body, causing pain during walking or standing.
Aging remains the most common cause of spinal stenosis. As people get older, the tissues in the spine change. Ligaments can thicken and become stiff. The cushioning discs between vertebrae lose water content and flatten. Joints may develop arthritis, causing bone to rub against bone. These changes happen to almost everyone over time, but they affect some people more than others.
When a spinal disc bulges or ruptures, the soft material inside can push into the spinal canal. This is called a herniated disc, and it directly reduces the space available for nerves. Bone spurs are another problem. These small, bony growths form when the body tries to repair damage from arthritis. While the body means well, these extra bits of bone often grow into the spinal canal and press on nerves.
Some people are born with a naturally narrow spinal canal. They may not have problems when young, but even small age-related changes can trigger symptoms earlier in life. Traumatic injuries from accidents, falls, or sports can also cause stenosis. Swelling from an injury may compress nerves immediately. Scar tissue that forms during healing can create long-term narrowing.
Stenosis symptoms depend on which nerves are affected. Many people experience pain radiating from the spine into the arms or legs. Numbness and tingling are also common, often described as a pins-and-needles sensation. Muscle weakness may develop over time as compressed nerves struggle to send proper signals. Some individuals notice their grip weakening or their feet dragging slightly when walking. Doctronic.ai can help people understand whether their symptoms might indicate stenosis and when to seek medical attention.
Neurogenic claudication is a specific symptom of lumbar stenosis. People with this condition feel pain, heaviness, or cramping in their legs when walking or standing. The discomfort typically improves when sitting down or leaning forward. This happens because bending forward slightly opens up space in the spinal canal. Many people find they can walk longer when pushing a shopping cart because the forward lean relieves pressure on their nerves.
Doctors start by asking questions about symptoms, when they started, and what makes them better or worse. They perform physical tests to check reflexes, muscle strength, and sensation. The doctor may ask the patient to walk, bend, or perform specific movements. These simple tests reveal a lot about which nerves might be affected.
Imaging tests confirm the diagnosis and show exactly where the narrowing occurs. X-rays reveal bone problems like spurs and arthritis, but cannot show soft tissues. MRI scans provide detailed pictures of discs, ligaments, and the spinal cord itself. CT scans provide excellent bone detail and can be combined with contrast administration for clearer nerve visualization. Doctors often use multiple imaging types together for a complete picture.
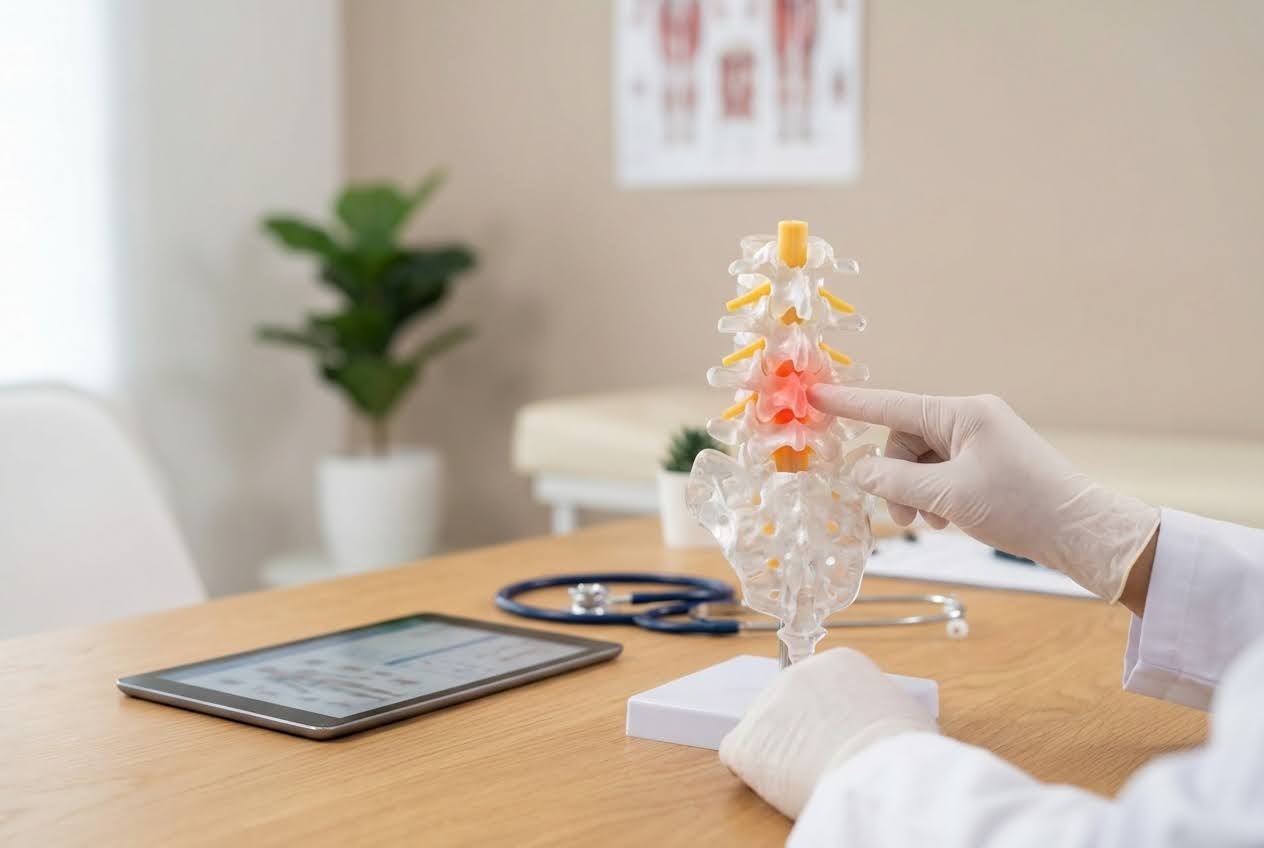 Non-Surgical Management and Therapy
Non-Surgical Management and TherapyPhysical therapy is often the first treatment recommended for stenosis. A therapist teaches exercises that strengthen core muscles supporting the spine. Stretching routines help maintain flexibility. Many patients learn specific positions that relieve pressure on compressed nerves. Regular exercise often significantly reduces symptoms without additional intervention.
Over-the-counter pain relievers like ibuprofen help manage mild symptoms. Doctors may prescribe stronger medications for more severe pain. Corticosteroid injections deliver anti-inflammatory medication directly to the affected area. These shots can provide relief lasting several weeks to a few months. While injections do not cure stenosis, they can make physical therapy more effective by reducing pain during exercises.
When conservative treatments fail, surgery becomes an option. Laminectomy is the most common procedure. The surgeon removes the lamina, the back part of the vertebra, to create more room in the spinal canal. This takes pressure off compressed nerves. Most patients experience significant pain relief after recovery.
Spinal fusion joins two or more vertebrae together permanently. Doctors recommend this when stenosis has caused spinal instability. Minimally invasive techniques use smaller incisions and special tools to perform surgery with less tissue damage. Recovery times are often shorter with these newer methods. Most people return to normal activities within several weeks to a few months after surgery.
Stenosis cannot be reversed, but symptoms can be managed effectively. Many people live normal, active lives with proper treatment. Surgery can provide long-lasting relief when other treatments fail.
High-impact activities like running or jumping may worsen symptoms. Exercises that arch the back, such as certain yoga poses, can increase pain. Walking and swimming are usually safe and beneficial.
Not necessarily. Some people have stable symptoms for years. Others experience gradual worsening. Early treatment and lifestyle changes can slow progression in many cases.
Seek medical attention when back pain includes numbness, weakness, or bladder problems. Pain that does not improve with rest or worsens over weeks also warrants evaluation.
Spinal stenosis is a narrowing of the spine that puts pressure on nerves, causing pain, numbness, and weakness. Most people manage this condition successfully through physical therapy, medications, and lifestyle changes, with surgery reserved for severe cases. For quick answers about spine-related symptoms, Doctronic.ai offers free AI doctor visits that provide personalized guidance based on the latest medical knowledge.
Meta Description: Understand why vaginal dryness during menopause occurs and explore effective treatments, from moisturizing therapies to low-dose estrogen and laser [...]
Read MoreMeta Description: Discover why perimenopause causes itching and explore effective relief strategies, from hormone therapy to skincare tips, to soothe dry and itchy skin.When [...]
Read MoreMeta Description: Understand why weight gain during perimenopause occurs and learn how to manage it through protein intake, resistance training, and better sleep habits.Why [...]
Read More